About Anaphylaxis
Important information about anaphylactic reactions*
Definition
Anaphylaxis is a severe, life-threatening allergic reaction that can occur within minutes of exposure to an allergen. It is a medical emergency that requires immediate treatment with epinephrine.

Epidemiology
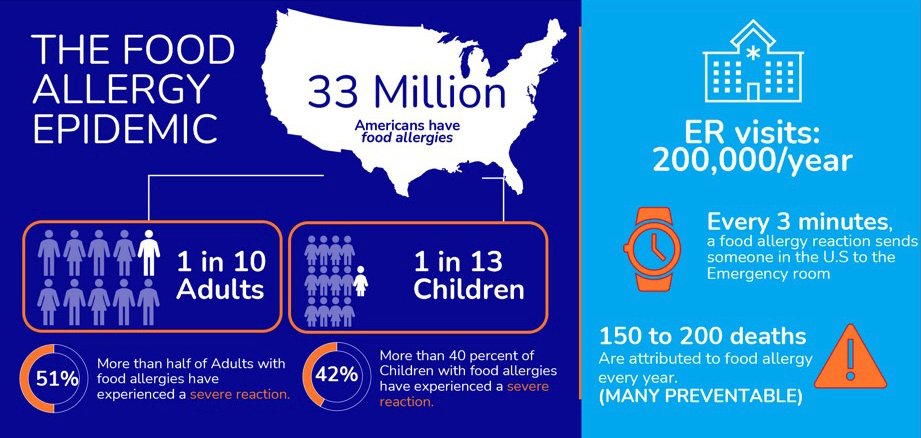
What causes anaphylaxis?
Anaphylaxis occurs when the body’s immune system overreacts to an otherwise harmless substance such as certain foods, insect stings, or medications.


Foods is the leading cause of anaphylaxis
The most common food allergies in the US are peanuts, tree nuts, shellfish, fish, milk, eggs, sesame, soy, and wheat.
Insect stings and bites
Stinging insects such as bees, wasps, hornets, yellow jackets, and fire ants can cause anaphylaxis. Certain tick bites can cause a person to develop delayed anaphylaxis after ingesting mammalian meat (known as Alpha-gal allergy).
Medicines are a major cause of anaphylaxis in adults
Common culprits include penicillin and other antibiotics, aspirin, and aspirin-related products and insulin.
Latex
Natural rubber latex may trigger a severe allergic reaction through direct contact or by inhaling small latex particles that have become airborne.
Physical activity
Exercise-induced anaphylaxis is a rare allergic reaction that occurs after vigorous physical activity in conjunction with certain foods.
Idiopathic
Sometimes the trigger for anaphylaxis is unknown and a reaction can occur at any time.
With proper evaluation, an allergist can help identify many causes of anaphylaxis and treatment options are available.
Symptoms
Symptoms typically involve more than one part of the body, such as the skin or mouth, the lungs, the heart, and/or the gut. Some examples include:
Hives, itching and swelling of the skin
Swelling of the lips, tongue or throat
Shortness of breath, cough or wheezing (whistling sound during breathing)
Dizziness and/or fainting
Stomach pain/cramping, bloating, vomiting, or diarrhea
Feeling like something bad is about to happen, anxiety or confusion
Knowing symptoms is key, and an anaphylaxis action plan guides you as to when treatment is needed. Below is an example of an anaphylaxis action plan.
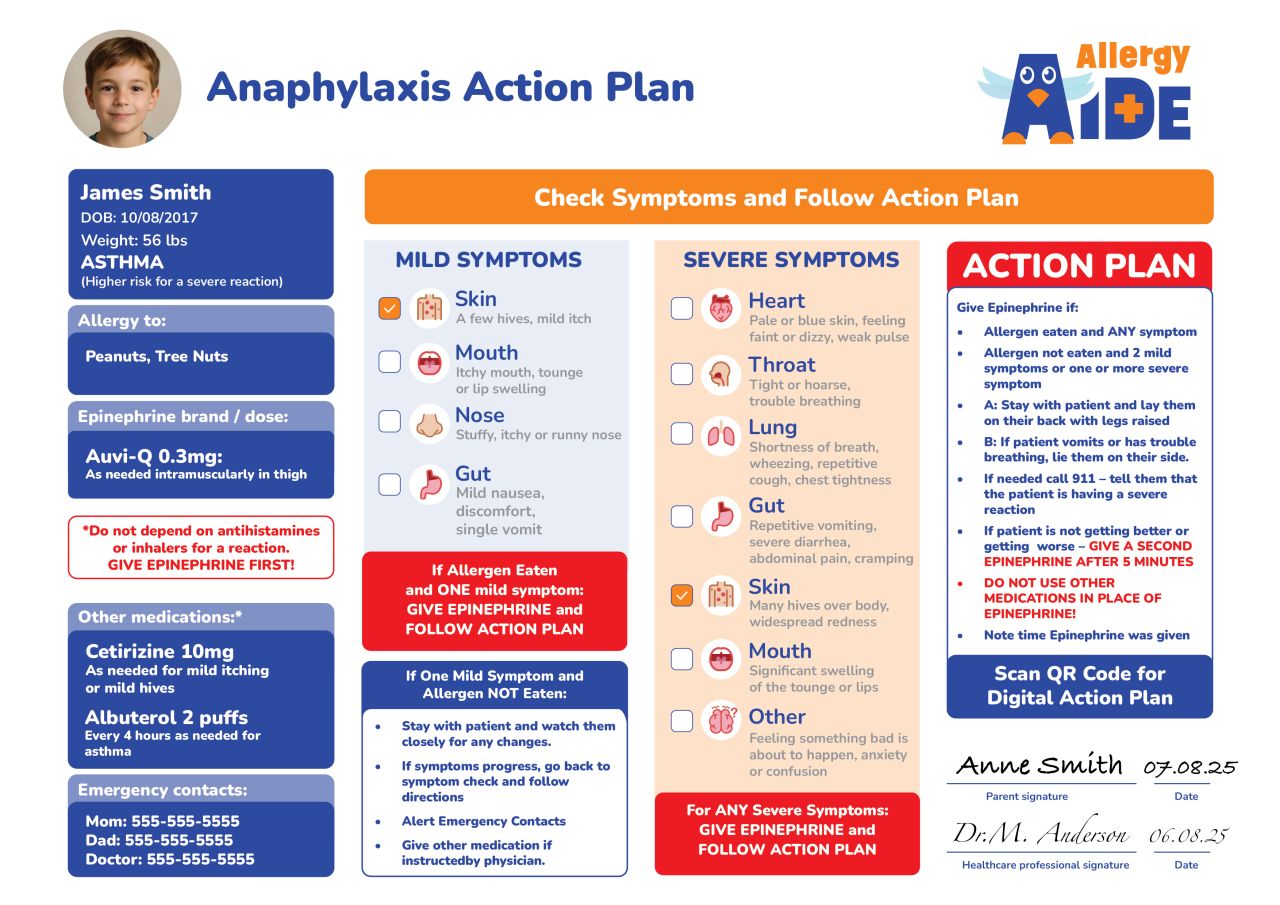
Epinephrine is the key to treatment
We say Epi-First, Epi-Fast as it is the only treatment for anaphylaxis (antihistamines and inhalers are not a replacement for epinephrine).
Prescription required
Epinephrine is only available as a prescription so ask your doctor. Make sure you review how to use the epinephrine device provided to you by the pharmacy as there are a number of different devices.
Early treatment is crucial
Early treatment of anaphylaxis provides the best chance to reverse and resolve these potentially life-threatening complications.
Carry two doses
It is recommended that two doses be carried at all times as a second dose may be needed if symptoms are not getting better or worsening.
Seek medical care
You may need to seek medical care / call 911 immediately – even if you feel better – because symptoms can recur.
Ask your doctor about other treatments, in addition to epinephrine.
Oral or Sublingual Immunotherapy (OIT or SLIT)
This is a treatment used by allergists that involves gradual oral introduction of an allergenic food over time to help decrease an individual’s sensitivity to that food.
Bee sting / Venom immunotherapy (VIT)
This is the gold standard for bee sting anaphylaxis and involves administering graded doses via injection under the skin over time to help with this allergy.
Drug allergy desensitization
An individual may be allergic to a medication that is required for treatment. An allergist can use this method to slowly give graded doses to allow this medication to be used.
Ask your doctor about these and other special treatments that may be available if you are at risk for anaphylaxis.
Early introduction of allergic foods
Early introduction of allergic foods (between the ages of 4 and 11 months) has been shown to reduce the risk of food allergy. Ask your pediatrician for guidance on proper introduction of foods for your infant.
Confirm your allergy
An accurate diagnosis is important. If you had symptoms of a reaction, whether to a food or a drug, an allergist can get a detailed history and may use skin testing and/or blood testing or challenges to help pinpoint the precise cause of you or your child’s reaction. An allergist can also use testing and challenges to see if you have outgrown your allergy.
Avoid your allergens
If you have a food allergy, be careful about everything you eat. Check ingredients on all food labels. Wash hands and use clean surfaces and utensils to prepare food. Ask restaurant staff how they prepare foods and carry a restaurant / chef card to show to your server.
Carry epinephrine with you at all times
Ensure that the epinephrine devices are up to date. Always carry two doses as a second one may be needed.
Prepare with a plan
Having an anaphylaxis action plan to prepare for a reaction is essential. Always have a plan on hand and review it regularly. Ask your doctor to help you create and review an anaphylaxis action plan.
Wear a medical ID bracelet or necklace
It lets others know of your allergy in an emergency. AllergyAIDE can also allow you to share your plan with other caregivers and a QR can give instant access to a custom action plan.
Ready to Create Your Anaphylaxis Action Plan?
AllergyAIDE makes it easy to create, maintain, and share your personalized anaphylaxis action plan with caregivers, schools, and healthcare providers.
*Information sourced from Kids with Food Allergies